
Simon Pendleton Quality Improvement and Podiatric Surgery Manager What is Normal Flat or High Arch Deformity Skin Condition Nails Circulation Sensation Who is normal Has anyone got a perfect foot ID: 909782
Download Presentation The PPT/PDF document "Recognising The Vulnerable Foot" is the property of its rightful owner. Permission is granted to download and print the materials on this web site for personal, non-commercial use only, and to display it on your personal computer provided you do not modify the materials and that you retain all copyright notices contained in the materials. By downloading content from our website, you accept the terms of this agreement.
Slide1
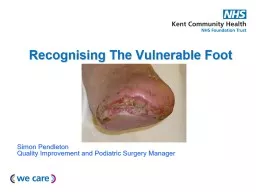
Recognising The Vulnerable Foot
Simon PendletonQuality Improvement and Podiatric Surgery Manager
Slide2What is Normal?
Flat or High ArchDeformitySkin ConditionNailsCirculationSensation
Slide3Who is normal?
Has anyone got a perfect foot?Who has flat feet?Who has high arched feet?
Slide4Deformity
Congenital : Syndactyly, Clawed Toes, Hallux Abducto Valgus (Bunions)Acquired : Broken Toes, Footwear Induced, Muscle or Nerve Injuries
Slide5Skin Conditions
The skin and its underlying tissues on the foot are liable to many problems from different sourcesMechanical stresses can cause: corns, callus and bursaeInfections: Bacterial, Fungal, ViralSweating Disorders: Hyperhidrosis, AnhidrosisChilblainsDermatological Conditions: Eczema, Psoriasis, Dermatitis
Slide6Nail Conditions
Involution (curling of the nail)Ingrowing Toe Nail (Onychocryptosis)OnychauxisOnychogryphosis (Rams horn)Paronychia (Inflammation of the tissues surrounding the nail)Onychomycosis (Fungal nail)
Slide7Slide8Slide9Fungal nails (Onychomycosis)
Treatment options:Topical Amorolfine (Loceryl nail lacquer)Oral Terbinafine (Lamisil)Conservative nail careSurgical nail care
Slide10Circulation: Common Problems
Vasospastic Disorders : Raynaud’s PhenomenonPeripheral IschaemiaVenous Problems : Varicose veins, Oedema
Slide11Sensation
As well as diabetes other disorders can reduce sensation to the lower limb including: Sciatica, Syphilis, Neurological disorders (Charcot Marie Tooth Disease)It can also be affected by vitamin B12 deficiency, trauma or excess alcohol consumption
Slide12Figures from NICEDiabetes is one of the most common chronic diseases in the UK and its prevalence is increasing.
In 2013, there were almost 2.9 million people in the UK diagnosed with diabetes. By 2025, it is estimated that more than 5 million people in the UK will have diabetes. In England, the number of people diagnosed with diabetes has increased by approximately 65% in the last decadeThe life expectancy of people with diabetes is shortened by up to 15 years, and 75% die of macro vascular complications.
Slide13How many people now have Diabetes in the UK?3,919,505
(Diabetes UK 2020)Estimated close to 4.8 million including undiagnosed people with undiagnosed Type 2 diabetes.5.3 million expected to be living with the condition by 2025.People with type 2 diabetes are 50% more likely to die prematurely.
Slide14Why the diabetic foot?Estimated £972m. - £1.13bn on healthcare related to foot ulceration and amputation in diabetes in 2014-15
equivalent to 0.72-0.83% of the entire NHS budget. Around two thirds of this expenditure was on care in primary, community and outpatient settings for ulceration. (DIABETIC FOOT CARE IN ENGLAND: AN ECONOMIC STUDY 2017)Foot ulcers precede up to 85% of amputations in Diabetic patients (Pecoraro 1990)Infection precedes 60% of amputations
Slide15People most at risk of amputationsType 1 Diabetes
Older people MenPeople living in the most deprived fifth of areas (>80% chance of an amputation than those in the least deprived fifth of areas)Lower risk of amputations:People from South Asian and Black ethnic backgrounds
Slide16NICE GuidancePublished: 26 August 2015, Updated January 2016, 11 October 2019
NG19 Diabetic foot problems: prevention and management https://www.nice.org.uk/guidance/ng19Most recent update includes antibiotic guidance for managing diabetic foot infections.
Slide17Commissioners and service providers should ensure that the following are in place:
A foot protection service for preventing diabetic foot problems, and for treating and managing diabetic foot problems in the community.A multidisciplinary foot care service for managing diabetic foot problems in hospital and in the community that cannot be managed by the foot protection service. Robust protocols and clear local pathways for the continued and integrated care of people across all settings, including emergency care and general practice. The protocols should set out the relationship between the foot protection service and the multidisciplinary foot care service.Regular reviews of treatment and patient outcomes, in line with the National Diabetes Foot Care Audit.
Slide18Assessing the risk of developing a diabetic foot problem
For adults with diabetes, assess their risk of developing a diabetic foot problemat the following times:When diabetes is diagnosed, and at least annually thereafterIf any foot problems arise.On any admission to hospital, and if there is any change in their status while they are in hospital.
Slide19Assessing the risk of developing a diabetic foot problem
When examining the feet of a person with diabetes, remove their shoes, socks,bandages and dressings, and examine both feet for evidence of the followingrisk factors:Neuropathy (use a 10 g monofilament as part of a foot sensory examination) Touch the toes test.Limb ischaemia (see the NICE guideline on lower limb peripheral arterial disease).Ulceration.Callus.Infection and/or inflammation.
Deformity.
Gangrene.
Charcot
arthropathy
.
Slide20Assess the person's current risk of developing a diabetic foot problem or needing an amputation using the following risk stratification
Low risk: no risk factors present.Moderate risk: At least 1 risk factor present.High risk: previous ulceration or amputation, on renal replacement therapy, or more than 1 risk factor present.Active diabetic foot problem: ulceration, spreading infection, critical ischaemia, gangrene, suspicion of an acute Charcot arthropathy, or an unexplained hot, red, swollen foot with or without pain.
Slide21Risk Factors to Consider & Identify
NeuropathyIschaemiaFoot deformityNail and skin problemsHistory of acute foot disease (High Risk)Compliance issues Impaired visionSmokingGlycaemic control
Impaired Renal function
Living alone
Slide22Risk Status Low RiskLow Risk
= No risk factors, no ischaemia or neuropathy 99% ulcer-free in following year (Leese et al 2006)No referral to Podiatry unless there is a foot problemAnnual review of foot assessmentLow “current” risk (not no risk!)64% of entire caseload likely to be Low Risk (Leese et al 2006)No Podiatry referral indicatedStructured Group education eg
DESMOND, X-PERT,
DERIK!
Slide23Low Risk Foot
Slide24Risk Status: Increased RiskIncreased Risk
= Mild neuropathy, ischaemia and/or risk factors Refer to GP/Podiatry for review every 3-6 months if appropriate or as agreed with patientRead codes for “Moderate risk” are used for this risk status23% of entire caseload likely to be Increased risk (Leese et al 2006)
Slide25Increased Risk Foot
Slide26Risk Status: High RiskHigh Risk
= Neuropathy and/or Ischaemia & combination of risk factors or history of acute foot disease eg ulcers, gangrene, amputations Refer to GP/Podiatry for review every 1-3 months or as agreed with patient13% of caseload likely to be high risk83 times more likely to develop foot ulcers than low risk group (Leese et al 2006)https://shop.diabetes.org.uk/store/literature/campaign-materials/red-card-foot-booklet.aspx
Slide27High Risk Feet
Slide28Risk Status: UlceratedUlcerated foot/Acute foot disease
= Urgent referral to Podiatry and multidisciplinary review according to care pathways4.7% of caseload likely to develop foot ulceration over 18 month period (Leese et al 2006)Estimated that 2-2.5% of the diabetes population has an ulcer in any given week, around 60,000-75,000 people in England. (DIABETIC FOOT CARE IN ENGLAND: AN ECONOMIC STUDY 2017)
Slide29Ulcerated Foot
Slide30Ulcerated Foot
Slide31GlycosolationA process in diabetes where the tissues undergo changes due to excessive glucose levels
Impairs the immune system, reduced resistance to infection. E.g., reduced chemotaxis, phagocytosis and intracellular killingReduced fibroplast proliferation and new tissue formation
Slide32Why Do People With Diabetes Develop Foot Problems?
Vascular DiseaseNeuropathy Infection
Slide33PAD/PVD/Macrovascular diseaseAtherosclerosis is accelerated and is more peripheral in diabetes
20x more common in people with diabetesMedial arterial calcification results in non-elastic arterial wallsReduction and stagnation of blood flow to the lower leg and foot causes ischaemia.NB Lower limb peripheral arterial disease: Diagnosis and management NICE CG147 - Issued: August 2012
Slide34Microvascular DiseaseBasement membrane thickening.
Decreased leukocyte migration.Increased viscosity of blood.Glycosylated haemoglobin decreases oxygen delivery to tissues.