
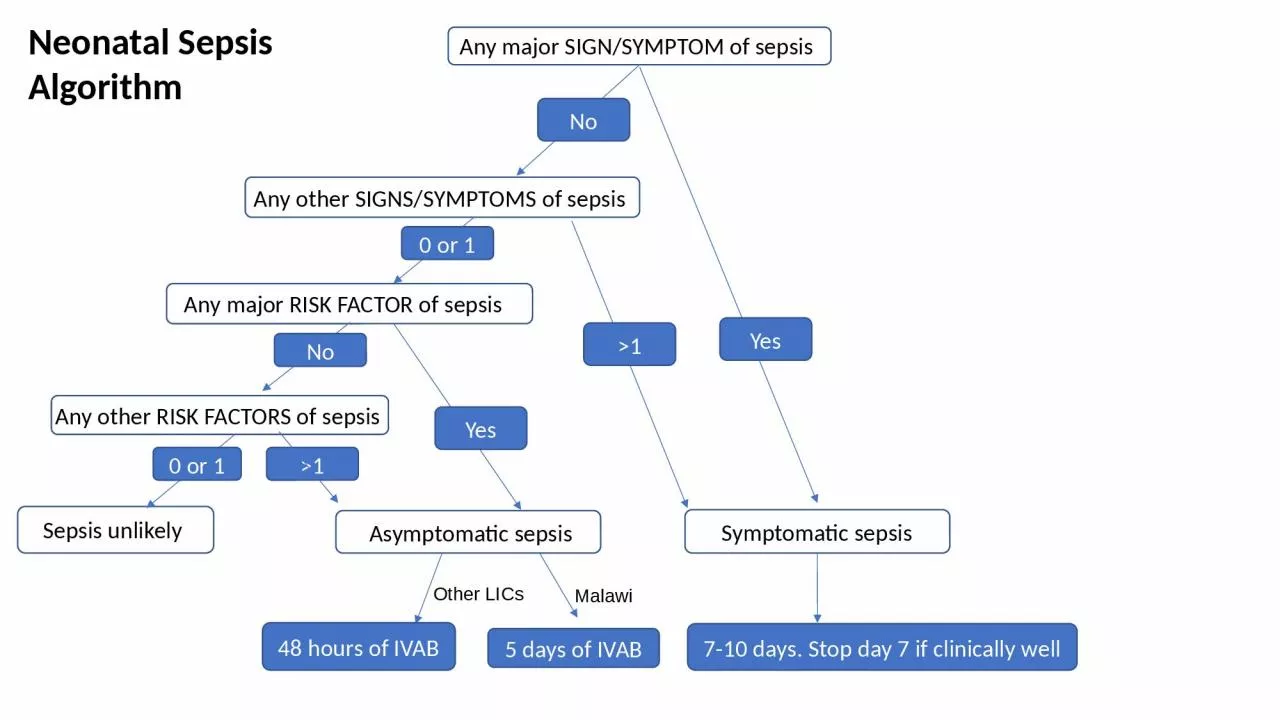
Any other SIGNSSYMPTOMS of sepsis Symptomatic sepsis Asymptomatic sepsis 48 hours of IVAB 710 days Stop day 7 if clinically well 5 days of IVAB Malawi Other LICs Sepsis unlikely A Any major RISK FACTOR of sepsis ID: 932782
Download Presentation The PPT/PDF document "Any major SIGN/SYMPTOM of sepsis" is the property of its rightful owner. Permission is granted to download and print the materials on this web site for personal, non-commercial use only, and to display it on your personal computer provided you do not modify the materials and that you retain all copyright notices contained in the materials. By downloading content from our website, you accept the terms of this agreement.
Slide1
Any major SIGN/SYMPTOM of sepsis
Any other SIGNS/SYMPTOMS of sepsis
Symptomatic sepsis
Asymptomatic sepsis
48 hours of IVAB
7-10 days. Stop day 7 if clinically well
5 days of IVAB
Malawi
Other LICs
Sepsis unlikely
A
Any major RISK FACTOR of sepsis
Any other RISK FACTORS of sepsis
Yes
No
>1
0 or 1
Yes
No
>1
0 or 1
Neonatal Sepsis Algorithm
Slide2Risk factors
MajorMaternal fever >38°C in
labour Prolonged rupture of membranes (PROM) >18 hours
Foul smelling amniotic fluidOther risk factors
<32/40 weeks gestation or <1500g (spontaneous labour only)
Signs/symptoms
MajorNeonatal temperature >37.5 °C
Boil/abscessGrunting/severe respiratory distress/ mod-severe WOB
LethargyUmbilical redness extending to the periumbilical skin or umbilicus draining pus
Deep jaundice: palms and soles of the baby deep yellowTachypnoea > 60 bpm
Convulsions/twitching or abnormal movementsMany or severe skin pustulesBilious vomiting with severe abdominal distension
Bulging fontanelle New onset of poor feeding
Not moving when stimulatedSwollen red eyelids with pus
Central cyanosisOther signs/symptoms
Pallor
Neonatal Sepsis Algorithm
Slide3Antibiotic doses
Gentamicin (IM/IV)
<7 days: 3 mg/kg (LBW) and 5 mg/kg (normal BW) per dose once a day
>7 days 7.5 mg/kg once a day Ampicillin (IM/IV)
<7 days: 50 mg/kg every 12 h >7 days every 8 h Benzylpenicillin (penicillin G) (IM)
<7 days: 50 000 U/kg every 12 h>7 days every 6 h
Supportive care
Thermoregulation: aim for 36.5-37.5 °CProvide respiratory support oxygen or CPAP as needed according to CPAP algorithm
Check blood glucose and provide feeding support as neededConsider 10ml/kg fluid bolus if shocked as per SHOCK algorithm
Consider 2.5mls/kg 10% dextrose if BS<2.5 mmol or 45 mg/dl – as per HYPOGLYCAEMIA algorithm
Neonatal sepsis management
Investigations
If possible
perform sepsis screen: FBC, CRP, blood culture
LP only for those who have clinical signs of meningitis (but stable) or late-onset neonatal sepsisAntibiotic choices
1st line: give local recommendationsIM/IV gentamicin and benzylpenicillin or
ampicillin 2nd line: If no improvement after 48 hours change to a third-generation cephalosporin
IV cloxacillin and gentamicin if greater risk of staphylococcal (skin infection).
Antibiotic duration (without investigations)Asymptomatic sepsis: T
reat for 48 hours and stop if well (Treat for 5 days in Malawi)Symptomatic sepsis: Stop at day 7 if clinically well otherwise continue for 10 days
Slide4Any one risk factor
Foetal distress
Resuscitation: Assisted ventilation >5 minutes or CPR >10 minutesApgar at 5 minutes <7
Any one sign or symptom
ComaConvulsions
LethargyHypotonia
Absent Moro reflexAbsent suck
Respiratory distress
No
Perform
Thompson score
to assess for HIE
No
Unlikely HIE
>37 weeks gestation
Consider
HIE but seek clinician review to confirm diagnosis
No
Yes
Hypoxic
Ischaemic
Encephalopathy Algorithm
Yes
Yes
Slide5Management page for HIE
Thermoregulation
Aim for normothermia
Avoid hyperthermia and hypothermia
Respiratory support
Give respiratory support as appropriate. Give oxygen if saturations <90% in air
Feeding
support, anticonvulsants and antibiotics
Give feeding support as appropriate1. Oral feeds (breast feed or bottle if breastfeeding is not possible)
2. Give NG feeds if BS <2.5mmol/L or <45mg/dL and not tolerating oral feeds3. Give IV fluids if BS <2.5mmol/L or <45mg/dL and not tolerating NG feed
If evidence of seizure activity give Phenobarbitone
as per convulsions algorithm.
Reassess suck, tone, coma, seizures every 8 hours for 72 hours in hospital
Treat for sepsis with antibiotics
Slide6Any one or more signs or symptoms of respiratory distress
Saturations in air <90%
Tachypnoea >60 bpm
Fever >37.5⁰C or <36⁰C and crepitations on auscultationGrunting
RecessionsAny increased work of breathingCyanosis
Apnoea
Respiratory Distress of the
Newborn
(RDN)
Unlikely RDN
No
Yes
Management
Respiratory Distress Algorithm
Slide7Teaching page
for RDN
Meconium aspiration
Consider if meconium stained amniotic fluid
Just because there was meconium at delivery doesn’t mean it was aspirated.
Most aspiration occurs in utero before the baby is born, so more likely if there was foetal distress in labour or has signs of birth asphyxia.
Floppy babies with severe HIE and meconium aspiration are unlikely to benefit from CPAP.
Transient tachypnoea of the
newborn (TTN)These babies are not unwell
RR is usually between 60-80 bpm and they don’t usually need oxygenThis should resolve in the first few hours of life.
TTN is more likely following elective C-section or a rapid vaginal delivery.Give antibiotics if unable to exclude other causes
i.e no chest xray
Respiratory distress syndromeConsider if < 37 weeks or diabetic mother
Benefit from CPAP see AlgorithmCongenital Pneumonia
Consider if temperature > 37.5 ⁰ c or < 36 ⁰ c and crepitations on auscultation
Risk factors for sepsis i.e maternal fever/PROM/foul smelling amniotic fluid
Management page RDN
Investigations
Perform a chest x-ray if it will change management
or if the infant is not
improving as expected or deteriorating.
Airway and respiratory support
Position airway
Give oxygen if oxygen saturations < 90% in air
If > 1kg consider CPAP according to CPAP algorithm
Feeding support
If breathing 60-80 bpm use cup/NGTIf needing CPAP use OGTIf breathing > 80bpm consider IV fluids
IV Access for Antibiotics
Give antibiotics including for suspected TTN (unless have chest x-ray and can safely exclude.)
Slide8Hypothermia
Mild = 36-36.4
°C
Mod = 32-35.9
°C
Severe = <32
°C
Hypothermia management page in
NeoTree
:
Warm the baby
S
kin to skinP
lace on warmer/resuscitaire
if unstable
Limit heat loss
Make sure the baby is dry
Put on a hat and wrap up the baby
If on the resuscitaire
put the sides up
Ensure room is free from drafts - windows and doors closed
MonitorRecheck
temperature every 30-60 minutes until normothermic
Watch out for overwarming
Complete NeoTree assessment to assess for signs of infection (consider if persistent hypothermia despite warming),
apnoea and
hypoglycaemia.
Temperature <36.4
°C?
Yes
No
Temperature >37.5
°C?
Yes
If fever persists follow NEONATAL SEPSIS algorithm
No
Normothermia
Recheck temp every 30-60 mins
Address any environmental causes: unwrap or remove baby from under
resuscitaire
Hypothermia Algorithm