PPT-Sergey Brodsky MD, PhD
SO
brambani
Published 2020-06-17 | 4924 Views
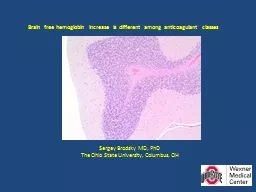
The Ohio State University Columbus OH Brain free hemoglobin increase is different among anticoagulant classes Anticoagulant therapy is the standard of care in patients
Download Presentation
Download Presentation The PPT/PDF document "Sergey Brodsky MD, PhD" is the property of its rightful owner. Permission is granted to download and print the materials on this website for personal, non-commercial use only, and to display it on your personal computer provided you do not modify the materials and that you retain all copyright notices contained in the materials. By downloading content from our website, you accept the terms of this agreement.
