PPT-Thyroid Disorders INTRODUCTION
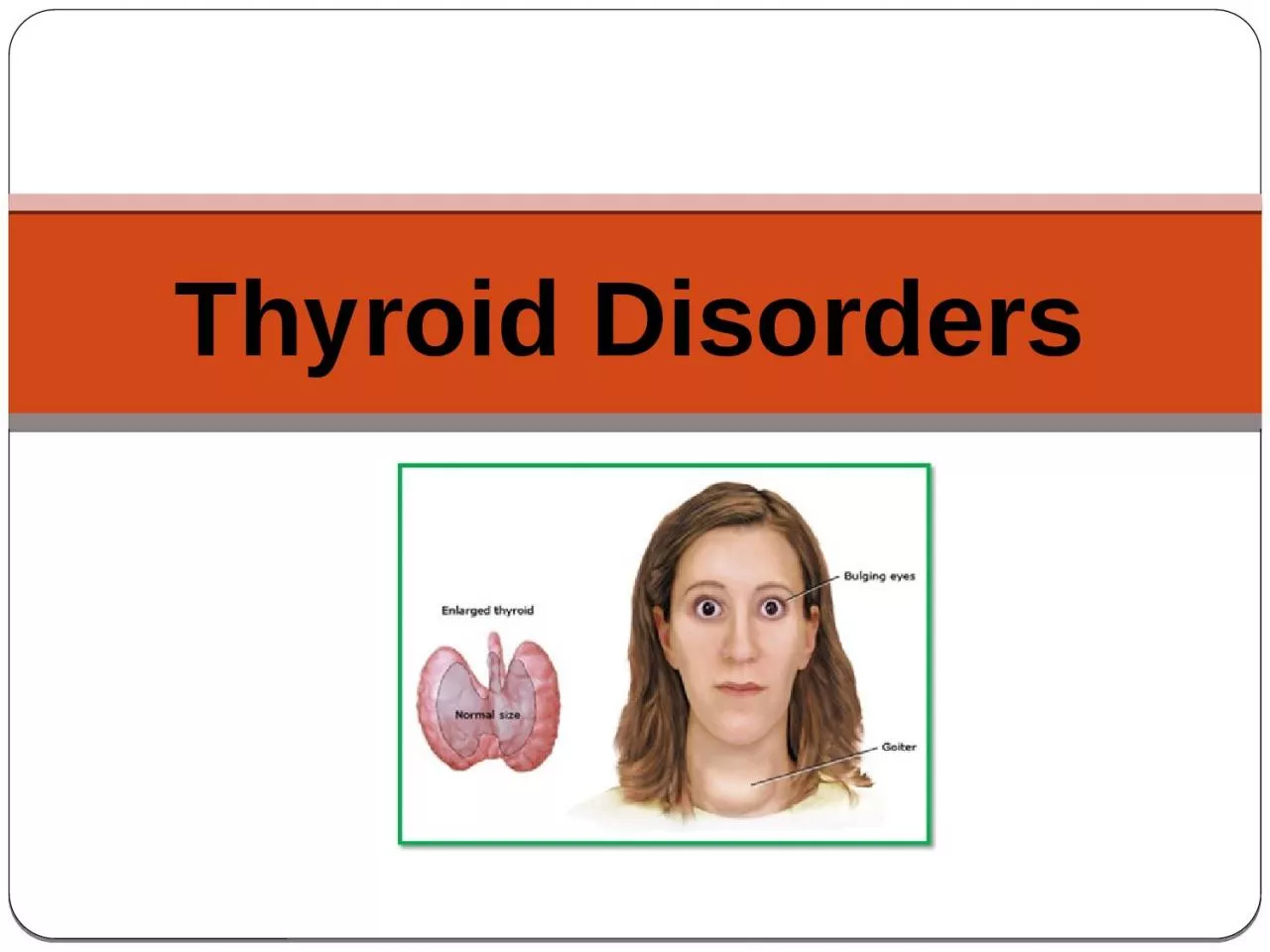
Thyroid rule In a child critical for normal growth and development In an adult maintain metabolic stability Thyroid disorders result in alterations in metabolic
Download Presentation
"Thyroid Disorders INTRODUCTION" is the property of its rightful owner. Permission is granted to download and print materials on this website for personal, non-commercial use only, provided you retain all copyright notices. By downloading content from our website, you accept the terms of this agreement.
Presentation Transcript
Transcript not available.