PPT-Integrating Telemedicine into Healthcare Delivery
Author : olivia-moreira | Published Date : 2019-06-22
Group 3 Final Project Kazi Russell Dave Seidman Rebecca Traina MEDINF 401DL American Healthcare System What is Telemedicine Definition The delivery of health care
Presentation Embed Code
Download Presentation
Download Presentation The PPT/PDF document "Integrating Telemedicine into Healthcare..." is the property of its rightful owner. Permission is granted to download and print the materials on this website for personal, non-commercial use only, and to display it on your personal computer provided you do not modify the materials and that you retain all copyright notices contained in the materials. By downloading content from our website, you accept the terms of this agreement.
Integrating Telemedicine into Healthcare Delivery: Transcript
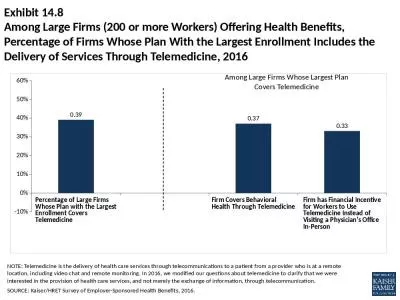
Group 3 Final Project Kazi Russell Dave Seidman Rebecca Traina MEDINF 401DL American Healthcare System What is Telemedicine Definition The delivery of health care services where distance is a critical factor by all . Telemedicine, May 9. , 2018. NATIONAL PERSPECTIVE. Presenting: Arvind K. Goyal, Medical Director. Terminology. Telemedicine. Telehealth. e-health. Online health. Virtual doctor visit. Tele-stroke. Tele-psychiatry etc.. Objectives:. Understanding the importance of broadband for telehealth. Explanation of the standards and safeguards. How it fits together for better healthcare. Broadband. Every facet of our daily life is touched by broadband and the Internet …. Jim Dickson. CEO . To maintain and support access to basic primary healthcare throughout Southern Cochise County by providing leadership and vision to address opportunities and challenges.. MISSION. SERVICE AREA. Patients as Consumers Customers of Healthcare What’s happening to healthcare … What is moving us along this paradigm… 2017 Trends New …now fear of regulatory changes Retail clinics ACA…and all its confusion and impacts What is Telemedicine?. A “virtual” doctor visit. The next phase of health care. Quality care. Convenient care. Cost effective care. 67%. of . Telemedicine . users . are . a. ges 21. . –. . 50. For Answers. Children’s Mercy Kansas City. The Highest Level of . Care for Kids. 40+ pediatric . specialty areas. Highest level pediatric trauma center. Highest level of neonatal intensive care unit. -May 15 2018Use of Telemedicine While Providing Medication Assisted Treatment MAT Under the Ryan Haight Act of 2008 where controlled substances are prescribed by means of the Internet the general requ Program Honoring those who use Information Technology to benefit societyFinal Copy of Case StudyLOCATIONSan Jose CA US YEAR2011STATUSLaureateCATEGORYHealthORGANIZATION International Virtual e-Hospital !. The latest on Telemedicine & what physician recruiters need to know about it. September 16. th. , 2015. Lew Benedict. Agenda . Defining Telemedicine. History . Successful Uses. Why It’s Growing and Where it’s Going. Ayushman. Bharat. Health and Wellness . Centres – Focus on Telemedicine (AP). 7.8.2019. Hyderabad, . Telangana. Health and Wellness Centres – Status of AP. . 2,167 . Health and Wellness centres are functioning in A.P. Objective: Explain the factors influencing health care delivery systems.. Factors That Influence Healthcare Delivery. Your assignment is to discuss with your group ways YOU THINK the factors on the next slide could influence the healthcare delivery system.. . Today, communicating with a friend in Japan is as easy and cheap as communicating with a friend across town, and families regularly use the Internet to keep in touch with far-flung relatives. . . Opportunities and Challenges". Dr.. . Lingaraj. . Niduvani. , . MSW, B.Ed., PGDWS, Ph.D.. Assistant Professor. , . Department Of Social Work, . Karnataka State Rural Development and . Panchayat. Raj University . NOTE: Telemedicine is the delivery of health care services through telecommunications to a patient from a provider who is at a remote location, including video chat and remote monitoring. In 2016, we modified our questions about telemedicine to...
Download Document
Here is the link to download the presentation.
"Integrating Telemedicine into Healthcare Delivery"The content belongs to its owner. You may download and print it for personal use, without modification, and keep all copyright notices. By downloading, you agree to these terms.
Related Documents