PPT-Pathway A Anti-TNFs in
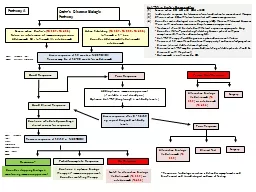
Crohns Disease used for Severe active CD HBI gt8 CDAI gt300 Inadequate response for tolerance of contraindication to conventional therapies Chronic active CD with
Download Presentation
"Pathway A Anti-TNFs in" is the property of its rightful owner. Permission is granted to download and print materials on this website for personal, non-commercial use only, provided you retain all copyright notices. By downloading content from our website, you accept the terms of this agreement.
Presentation Transcript
Transcript not available.