PPT- Cardiovascular System - Ch 11
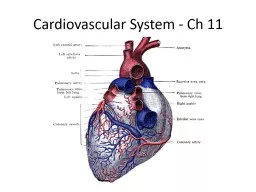
Heart Facts heart pumps 7000 liters of blood daily heart arteries arterioles capillaries site of gas waste nutrient exchange venules veins heart 14 cm long x 9 cm
Download Presentation
" Cardiovascular System - Ch 11" is the property of its rightful owner. Permission is granted to download and print materials on this website for personal, non-commercial use only, provided you retain all copyright notices. By downloading content from our website, you accept the terms of this agreement.
Presentation Transcript
Transcript not available.